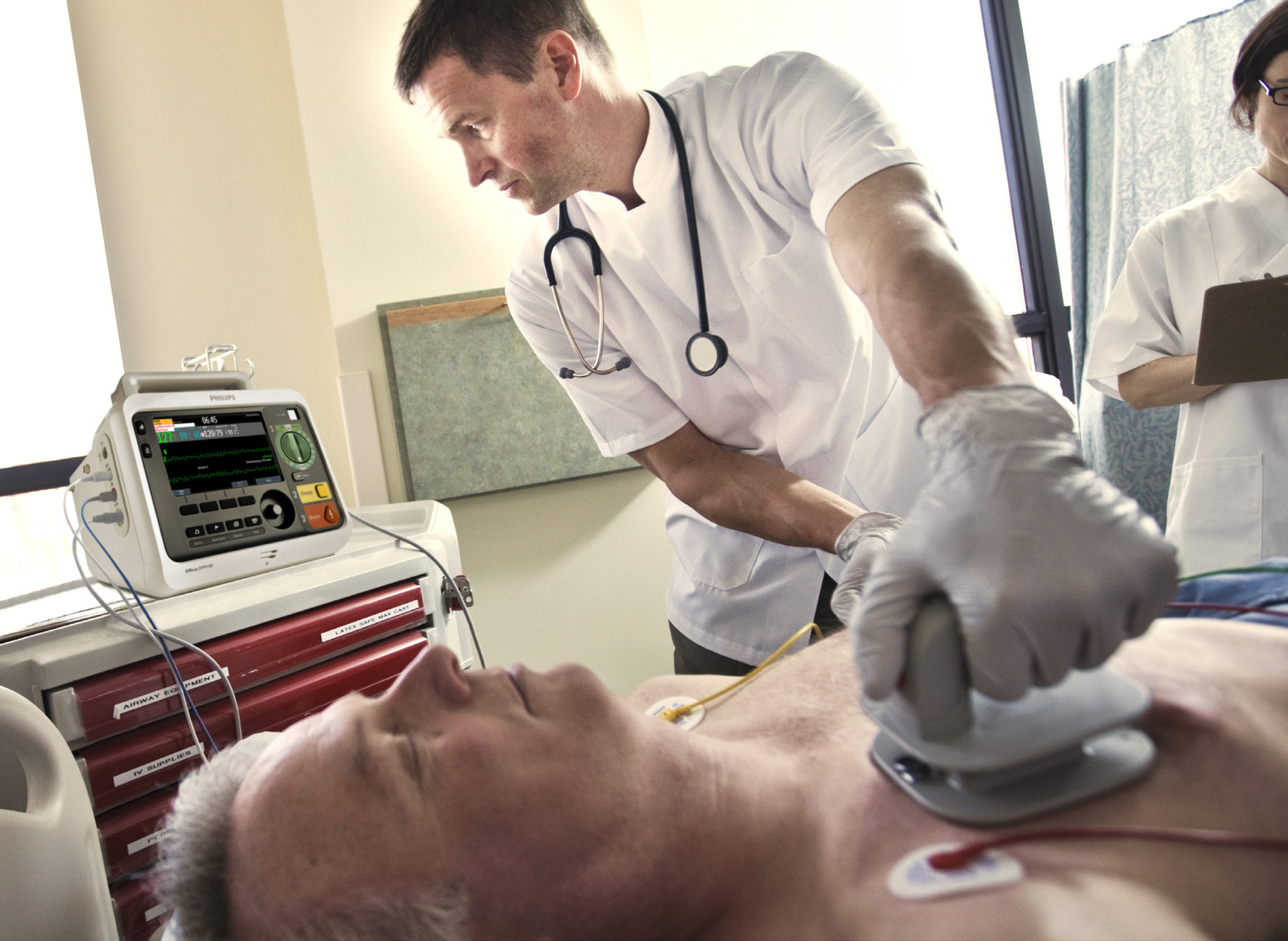
The main causes of death from heart disease include heart failure and malignant arrhythmias caused by ventricular fibrillation. Results from the RAFT trial, published in NEJM in 2010, showed that the combination of an implantable cardioverter defibrillator (ICD) plus optimal drug therapy with cardiac resynchronization (CRT) significantly reduced the risk of death or hospitalization for heart failure. However, with only 40 months of follow-up at the time of publication, the long-term value of this treatment strategy is unclear.
With the increase of effective therapy and the extension of use time, the clinical efficacy of patients with low ejection fraction heart failure has been improved. Randomized controlled trials typically evaluate the effectiveness of a therapy for a limited period of time, and its long-term efficacy can be difficult to assess after the trial is over because patients in the control group may cross over to the trial group. On the other hand, if a new treatment is studied in patients with advanced heart failure, its efficacy may soon become apparent. However, starting treatment early, before symptoms of heart failure are less severe, may have a more profound positive impact on outcomes years after the trial ends.
The RAFT (Resynchronisation-Defibrillation Therapy Trial in Ambed Heart Failure), which evaluated the clinical efficacy of cardiac resynchronisation (CRT), showed that CRT was effective in most New York Heart Society (NYHA) Class II heart failure patients: with an average follow-up of 40 months, CRT reduced mortality and hospitalization in patients with heart failure. After a median follow-up of nearly 14 years in the eight centers with the largest number of enrolled patients in the RAFT trial, results showed continued improvement in survival.
In a pivotal trial involving patients with NYHA grade III or ambulate grade IV heart failure, CRT reduced symptoms, improved exercise capacity, and reduced hospital admissions. Evidence from the subsequent heart Resynchronization – Heart Failure (CARE-HF) trial showed that patients who received CRT and standard medication (without an implantable cardioverter defibrillator [ICD]) survived longer than those who received medication alone. These trials showed that CRT alleviated mitral regurgitation and cardiac remodeling, and improved left ventricular ejection fraction. However, the clinical benefit of CRT in patients with NYHA Grade II heart failure remains controversial. Until 2010, results from the RAFT trial showed that patients receiving CRT in combination with ICD (CRT-D) had better survival rates and fewer hospitalizations than those receiving ICD alone.
Recent data suggest that direct pacing in the left bundle branch region, rather than placement of CRT leads through the coronary sinus, can yield equal or better results, so the enthusiasm for CRT treatment in patients with mild heart failure may be further heightened. A small randomized trial using this technique in patients with CRT indications and a left ventricular ejection fraction of less than 50% showed a greater likelihood of successful lead implantation and greater improvement in left ventricular ejection fraction compared to patients who received conventional CRT. Further optimization of pacing leads and catheter sheaths can improve the physiological response to CRT and reduce the risk of surgical complications.
In the SOLVD trial, patients with symptoms of heart failure who took enalapril survived longer than those who took placebo during the trial; But after 12 years of follow-up, survival in the enalapril group had dropped to levels similar to those in the placebo group. In contrast, among asymptomatic patients, the enalapril group was no more likely to survive the 3-year trial than the placebo group, but after 12 years of follow-up, these patients were significantly more likely to survive than the placebo group. Of course, after the trial period was over, ACE inhibitors were widely used.
Based on the results of SOLVD and other landmark heart failure trials, guidelines recommend that medications for symptomatic heart failure be started before symptoms of heart failure appear (stage B). Although patients in the RAFT trial had only mild symptoms of heart failure at the time of enrollment, nearly 80 percent died after 15 years. Because CRT can significantly improve patients’ heart function, quality of life, and survival, the principle of treating heart failure as early as possible may now include CRT, especially as CRT technology improves and becomes more convenient and safe to use. For patients with low left ventricular ejection fraction, it is less likely to increase the ejection fraction with medication alone, so CRT can be initiated as soon as possible after diagnosis of left bundle branch block. Identifying patients with asymptomatic left ventricular dysfunction through biomarker screening could help advance the use of effective therapies that could lead to longer, high-quality survival.
It should be noted that since the initial results of the RAFT trial were reported, there have been many advances in the pharmacological treatment of heart failure, including enkephalin inhibitors and SGLT-2 inhibitors. CRT can improve cardiac function, but does not increase cardiac load, and is expected to play a complementary role in drug therapy. However, the effect of CRT on the survival of patients treated with the new drug is uncertain.
Post time: Jan-27-2024